- +917892951808
- Indiranagar, Bangalore
Best Dental Clinic In Bangalore Indiranagar | Best Dentist in Bangalore Indiranagar
- Home
- About Us
- Treatments
- Blog
- Contact Us
About US
Best Dental Clinic in Indiranagar, Bangalore
Center for dental implants and laser dentistry
Dental Solutions clinic in Indiranagar is Bangalore’s leading provider of dental cosmetic and therapeutic treatments, considered as the best dental clinic in Bangalore. We have few of the Best dentists in Bangalore who provide comprehensive patient care in the quickest time possible. The top dental clinic in Bangalore has a dedicated team of professional and administrative staff primarily to cater to international patients. Dental Solutions’ international patient care department receives patients from Europe, the United States, UAE, the Far East, and other parts of the world to provide quality healthcare services.
0
k
Tooth Extraction
0
k
Implants Placed
0
k
Root Canal
Why Choose Us
Best Dental Clinic in Bangalore That You Can Trust
We are the premier choice for all your dental needs. Trust us to help you achieve a healthy and beautiful smile.
Dentist
Consult with the best Dentists in Indiranagar, Bangalore

DR RAMYA DS, BDS (GOLD MEDAL), MDS
Prosthodontist, Implantologist & Laser Practitioner (LAHA- Slovenia) Certified Practitioner Digital Smile design & Certified Practitioner Clear Path, Diploma & Master – University of Vienna, Austria
DR. BALASUBRAMANYA K V, BDS, MDS
Professor and Senior Consultant Department of Periodontics Diploma and Master (SOLA) at the University of Vienna Austria.
Soft and Hard Tissue Laser (LAHA) Slovenia

Our Dental Services
Best Dental Clinic Treatments
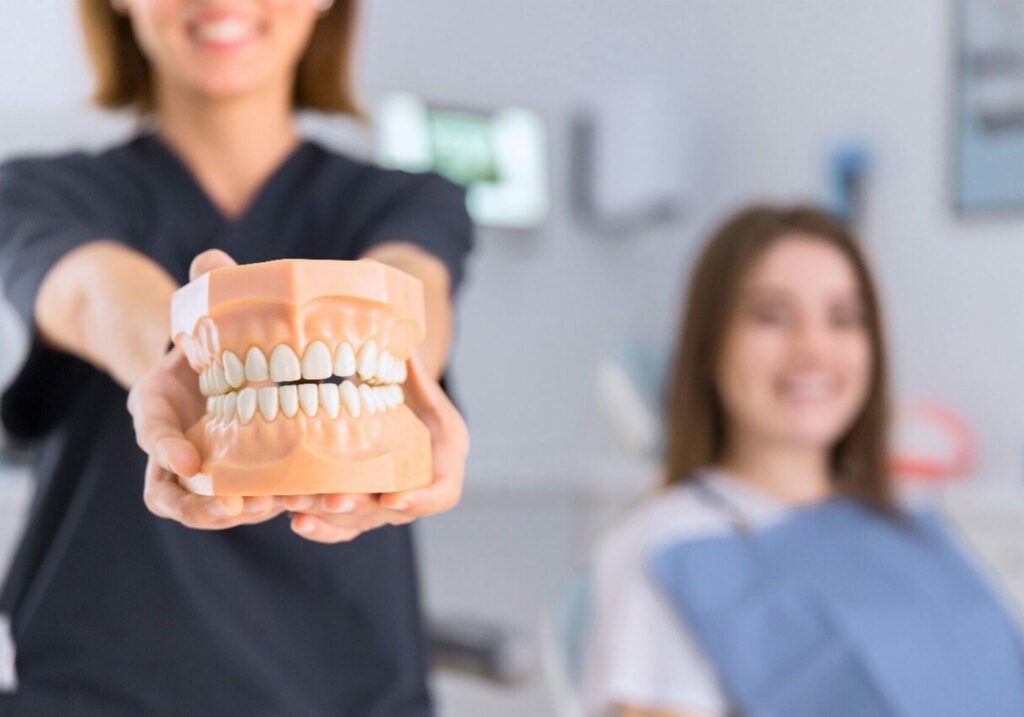
Treatments
Dental Services
Treatments
Laser Assisted Treatments
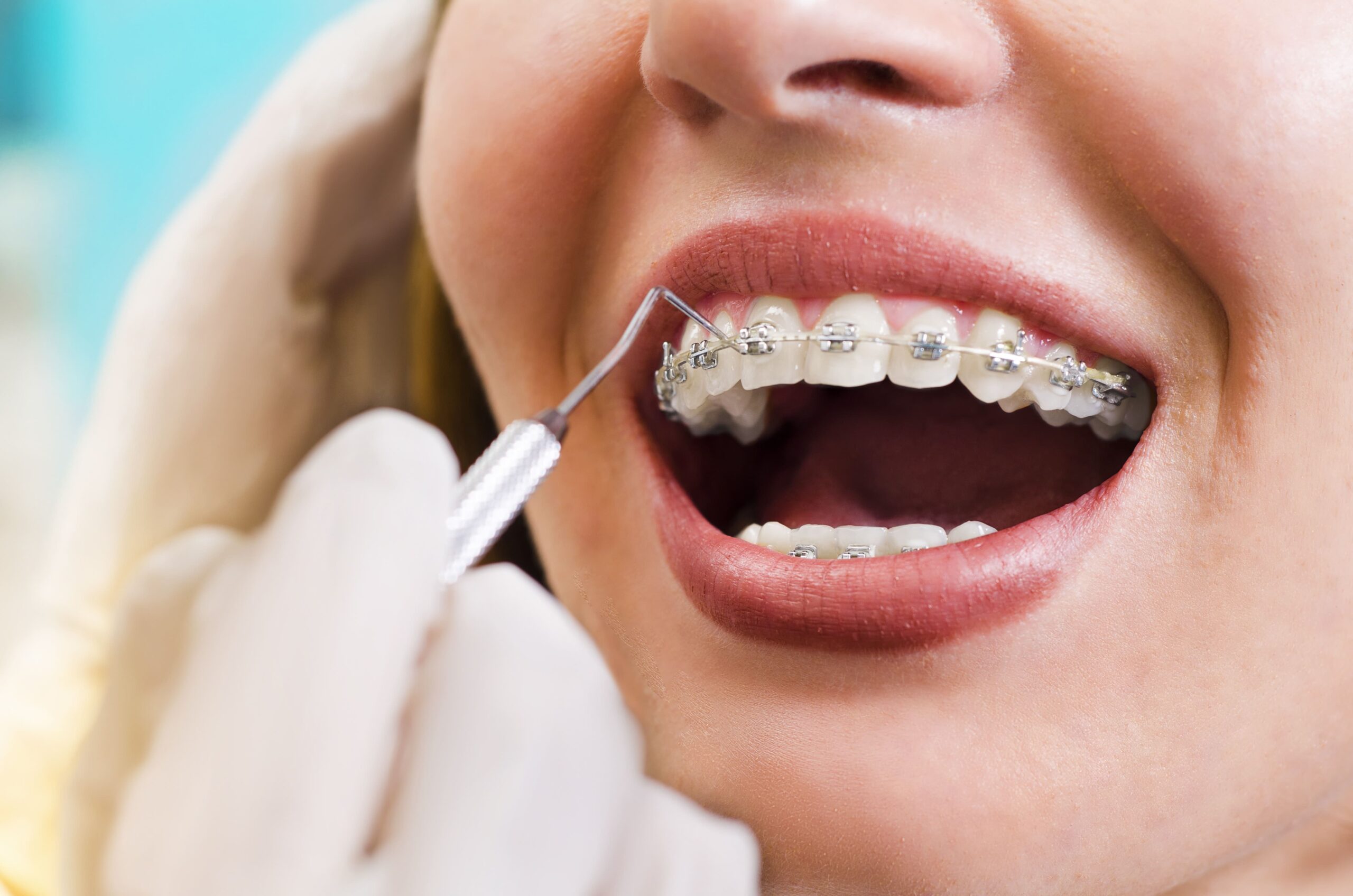
Treatments
Endodontic Treatments

Treatments
Invisalign® braces
Treatments
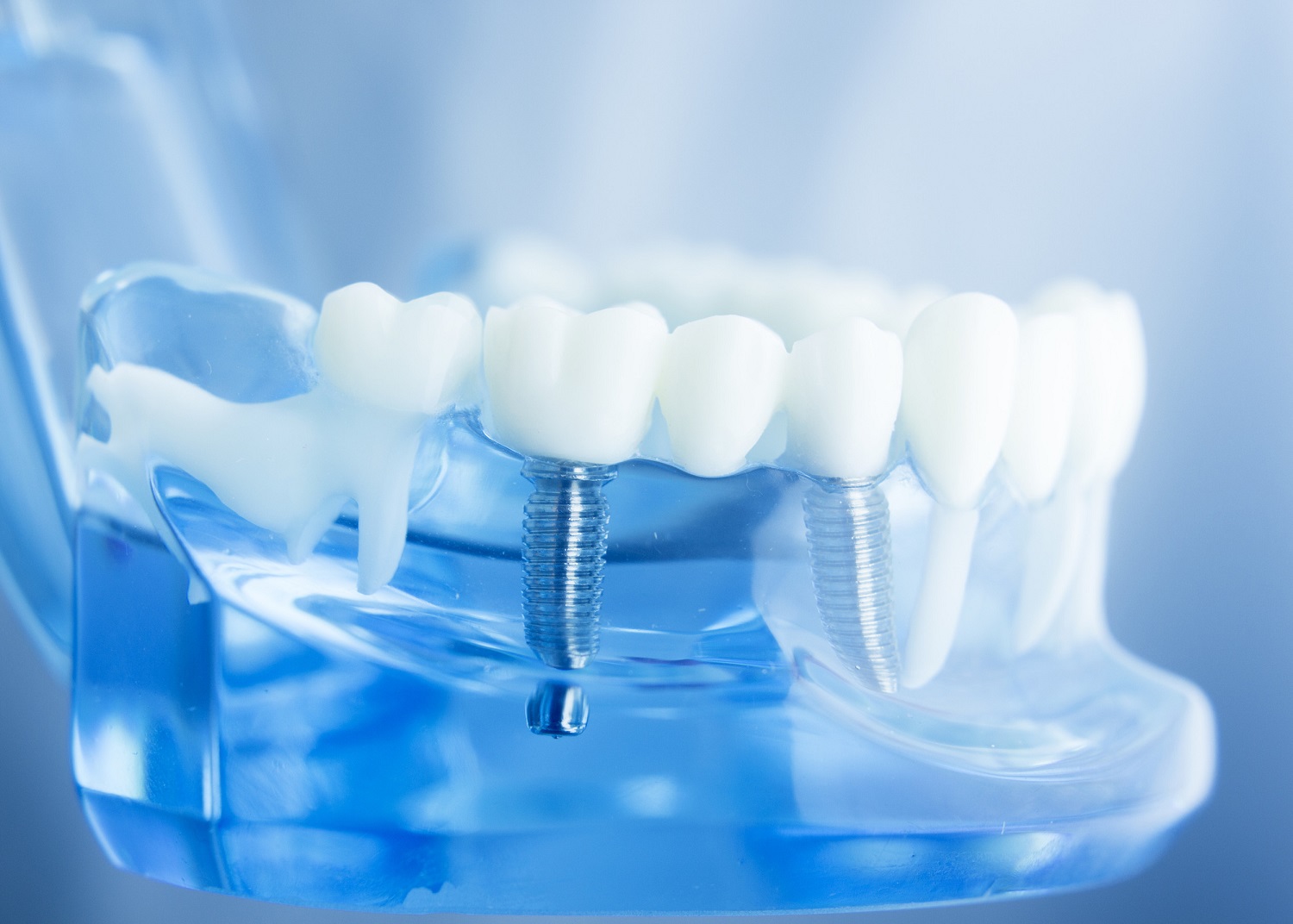
Dental Bridges
Treatments
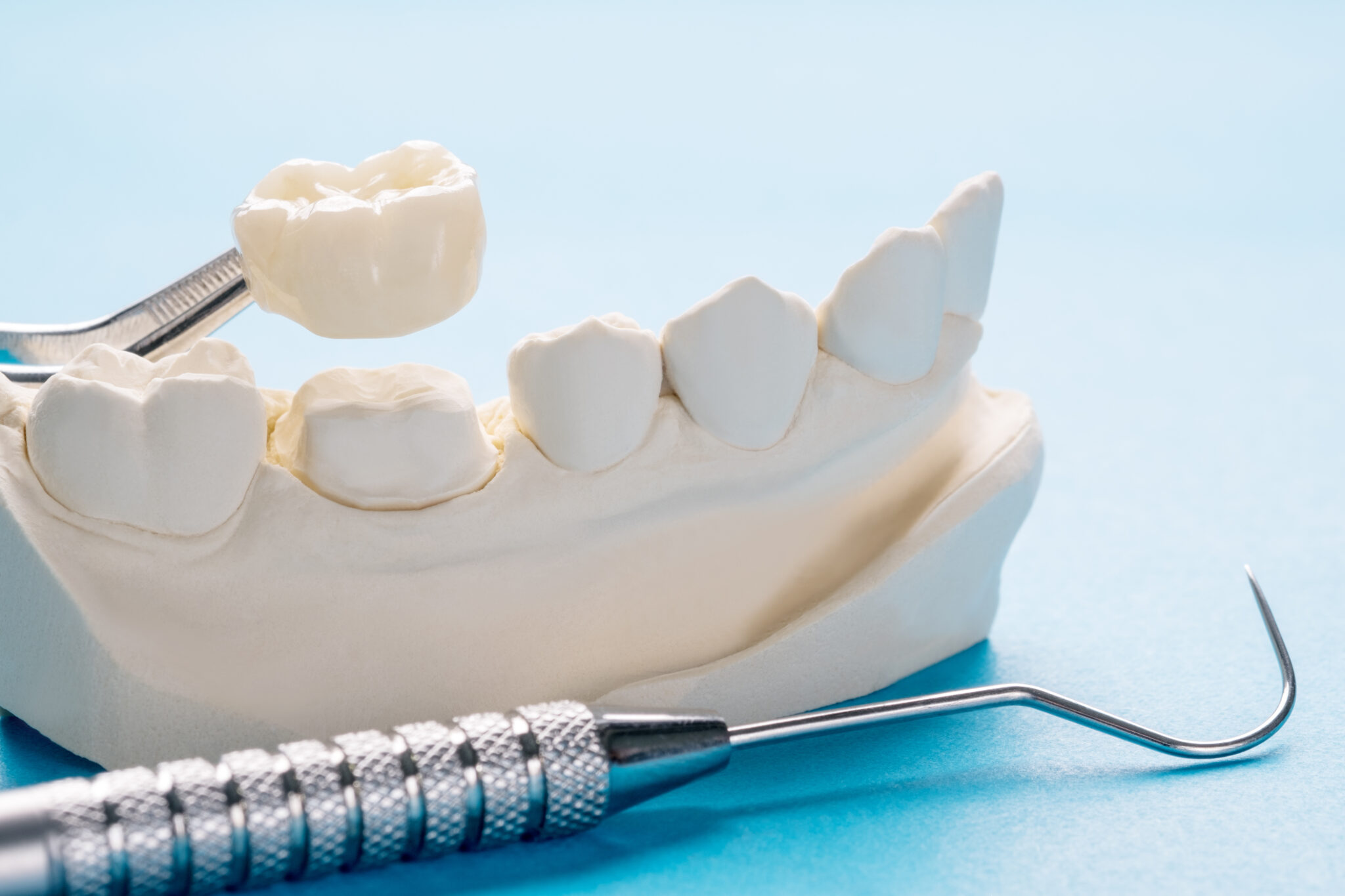
Dental Crown

Treatments
Dentures
Treatments
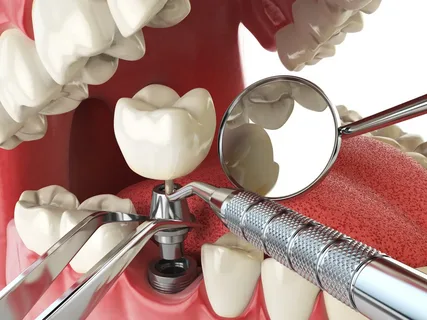
Dental Implants

Treatments
Digital Smile Design
Treatments
Full Mouth Rehabilitation
Treatments
Gentle Ray – Dental Caries-Diagnosis

Treatments
Invisible Orthodontics – Clear Path
Treatments
Dental Treatment Costs in Bangalore
Get In Touch
Experience painless dentistry and expert dental care like never before!
Experience painless dentistry and expert dental care like never before – from first visit to final result, our gentle approach and skilled doctors will keep you smiling!

At our clinic, we know that trust is the key to building a long-lasting relationship with our patients. That’s why we go above and beyond to ensure that you feel comfortable and confident in our care.
Patient Testimonials and Reviews
"It is testimonials like these that brighten our smile. Irshad Ahmed from Canada visited our dental clinic in Bangalore for periodontal treatment, he initially suffered from the consequences of the gum disease, but after the treatment, he is happy and completely relieved of the pain and the treatment has already started showing great results. Watch… "

Irshad Ahmed
Root Canal
"Ibrahim a pilot from the Maldives shares his experience after undergoing Wavelength Optimized Periodontal Therapy (WPT) and LANAP, Laser Assisted New Attachment Procedure at Dental Solutions Clinic in Bangalore. [vc_video link=”https://youtu.be/ne4loPmOBHM”] Wavelength Optimised Periodontal Therapy is used to treat Periodontal diseases. The word “periodontal” means “around the teeth”. A periodontal disease is caused by Gram-Positive… "

Ibrahim
Periodontal
Parthapradhan recently underwent a Wavelength Optimized Periodontal Therapy (WPT) for treating periodontitis at Dental Solutions Bangalore. Treatments for Periodontal diseases range from nonsurgical to surgical. Non-surgical treatment would include cleaning, scaling and root planning whereas surgical would include Flap surgery, pocket reduction surgery, bone or tissue grafting, guided tissue regeneration and bone surgery. Dentists now…

Parthapradhan
Wavelength Optimised Periodontal Therapy
Hi, my name is Anirudh. This is my second visit back to see Dr. Balu. My first time was about five years ago when I was living in the US. I got my WPT treatment done for my gums. Being very satisfied with that, I decided to visit again now post Covid at the new clinic with all the new staff and much better equipment. So this time I needed a replacement of nine crowns, which I had 15 years ago done when I was a kid. They all needed to be replaced, and in the meantime we found cavities that had formed around some of the old crown gaps. So Dr. Ramya did a lot of the Crown replacement and the fillings, while Dr. Balu handled the depigmentation of my gums that I wanted to have done, as well as some teeth bleaching and the gum cleaning, similar to what I had done before.

Anirudh
Wavelength Optimised Periodontal Therapy
Blogs
Our Latest Blogs

Deciphering the Ideal Age for…
Deciphering the Ideal Age for Kids to Get Braces Orthodontic treatment for kids is not just about achieving a picture-perfect...
Read More
Why choose a pediatric dentist…
Why choose a pediatric dentist instead of a general dentist? Choosing the right dentist for your child can be a...
Read More
What causes bumps in gums…
What causes bumps in gums after a root canal? How do you treat it? What is a Gum Boil? A...
Read More
Root Canal Treatment: Understanding Diagnosis,…
Root Canal Treatment: Understanding Diagnosis, Procedure, and Potential Side Effects Root canal treatment is a common dental procedure that is...
Read More
Do I Need to See…
Do I Need to See a Dentist for Swollen Gums? Swollen gums can range from a minor irritation to a...
Read More
The Surprising Connection Between Oral…
The Surprising Connection Between Oral Health and Overall Well-being Oral health is an often overlooked aspect of overall well-being, but...
Read More